A. Metabolic effects of low glycaemic-index diets
Observational studies indicate that the GI of the diet may be an important determinant of metabolic risk. The major sources of carbohydrate in the Western diet (highly-refined cereal and potato products) tend to have high GI values, which has been linked to the widespread occurrence of type 2 diabetes and CVD [23].
GI has been shown to be positively associated with the prevalence of the metabolic syndrome and insulin resistance in a cross -sectional study of 2834 subjects from the Framingham Offspring cohort [24]. Odds of having metabolic syndrome were reported to be 41% higher in the highest quintile of dietary GI compared with the lowest quintile (median GI values 84 and 72 respectively), and insulin resistance was found to be increased across quintiles (p < 0.001) [23].
Associations have also been reported between GI and both unfavorable lipid profiles and raised inflammatory status. In 280 women aged 45–70 years from the Nurses Health Study fasting triacylglycerol levels were shown to be positively related to GI [25]. Serum HDL levels have been found to be negatively related to GI in 1420 subjects aged 18–64 years from the 1986–7 Survey of Britain Adults 18–64 years [26], in which GI was the only dietary factor found to be significantly associated with HDL levels in multiple linear-regression analysis. Plasma levels of high-sensitivity C-reactive protein, a sensitive marker of systemic inflammation, were found to be positively associated with both GI and GL in 244 women from the Nurses' Health Study, aged 45–82 years, with a stronger relationship in overweight women than in normal-weight women [27].
Fig. 1. Low GI diets and metabolic syndrome.

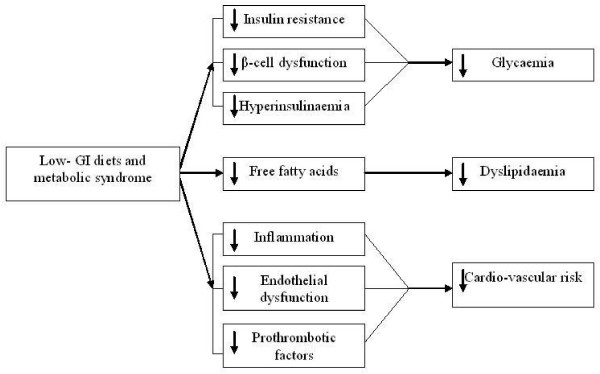
Description: Low GI diets decrease insulin resistance and insulin levels, causing plasma glucose reduction, decrease free fatty acids levels, inflammation and endothelial dysfunction, causing an important reduction of cardiovascular risk factors.
Weight loss is an additional potential mechanism by which low-GI diets may contribute to reduced risk of metabolic syndrome.
Induction of a rapid initial weight loss with low-carbohydrates diets may be partly explained by a reduction in overall caloric intake, which may be the result of a great limitation of food choices by the requirements of minimizing carbohydrates intake [28,29], to the initial increase in circulating β-hydroxybutyrate, which may suppress appetite [30] and to the satiating effect of low-carbohydrates diets containing relatively high amounts of protein [31,32]. Some of the initial weight loss may also be explained by a reduction of glycogen stores from liver (5% of liver weight) and muscle (1% of muscle weight). Each gram of glycogen is stored with approximately 3 g of water [33]. Therefore a weight loss of 1–2 kg can theoretically be achieved within the first week of the diet because of substantial glycogen reductions in liver and muscle and excretion of the liberated water in urine [15]. Depending on the rate of glycogen depletion, this process may last up to 7–14 days, after which weight loss slows [34]. It should be noticed in this respect that loss of glycogen and water is not a true measure of weight loss, as their stores will be replenished once the diet is stopped [15].



